Daniel Diaz, DO, thinks everyone deserves a second chance. As the son of Mexican immigrants, he witnessed firsthand how a fresh start can make a...
… As I sit down to write these words, my heart swells with emotions, memories, and a sense of gratitude that has accompanied me on...
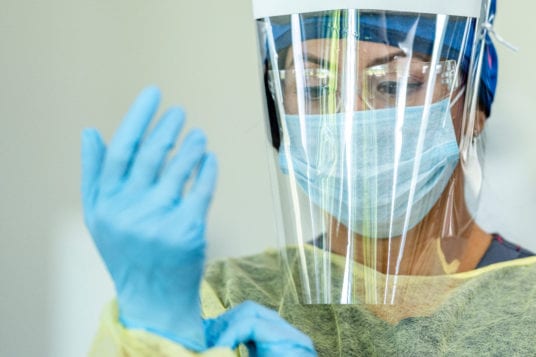
As a front-line worker in the health care sector, your safety is of the utmost importance when treating patients. Learn more about the importance of PPE in nursing.
Forensic psychology is an exciting field that intertwines psychology with understanding the law. To embark on this path, understanding the forensic psychology license requirements is...
Last year, we conducted a research study focused on gaining a deeper understanding of the effectiveness of play-based and trauma-informed teaching practices at an early...
Australian sociologist Judy Singer coined the term “neurodiversity” in 1998 when she was writing her undergraduate thesis at the University of Technology, Sydney. In it,...
Pooja Behl Luthra has never thought about an end point to her learning and education. To her, lifelong learning doesn’t only expand her thinking. It...
Career Development
Forensic psychology is an exciting field that intertwines psychology with understanding the law. To embark on this path, understanding the forensic psychology license requirements is crucial. This guide will lead...
Forty percent of Americans with mental disorders cannot access mental health services, particularly pharmacotherapy. A program at The Chicago School of Professional Psychology seeks to change that.
Here is everything you need to know about how to get started as a Certified Clinical Mental Health Counselor.
Our community is full of practical altruists—those who are driven to make a difference, while still making a stable living for themselves and their families.